The illusion of control refers to people’s inclination to overestimate their power to control events. It was named by Ellen Langer, a psychologist from the United States, and is thought to impact gambling behavior and paranormal beliefs. The illusion of control, like illusory superiority and optimism bias, is a positive illusion. The illusion could arise…
Egocentric Bias: How Personal Perspective Skews Judgment
Egocentric bias is a cognitive bias that influences one to rely too heavily on their own perspective and experiences when evaluating events surrounding them, as well as the feelings and behaviors of others. Individuals with an egocentric bias may believe others share the same opinion as they do. This illusion of transparency can lead to misunderstandings, as it assumes…
New Drug Molecule Inhibits Stress Hormone Receptor Activity
Stress is not just an oppressive feeling encountered when one is overburdened; rather, it constitutes the body’s inherent response to acute or persistent strain. The stress response is responsible for facilitating prompt adaptation to peril or changes in circumstances. However, should this physiological reaction — vital for survival — escalate and persist indefinitely, it can…
Superior Colliculus More Important for Vision Than Previously Thought
Researchers at the Netherlands Institute for Neuroscience discovered that the superior colliculus, a brain area preserved through evolution, is more important for vision than previously thought. Upon visual inspection, an object can be readily differentiated from the surrounding context. Despite the apparent simplicity of this, the manner in which our brain achieves it remains quite…
Restoring Mitochondrial Synapse Connections to Treat Alzheimer’s Disease
Nerve cells in the brain require an immense quantity of energy to maintain their connections for communication with other nerve cells and to survive. Energy production is impaired in Alzheimer’s disease, and synaptic connections eventually deteriorate and fail, resulting in the loss of new memories. A Scripps Research team has now identified the energetic reactions…
What is the Bias Blind Spot?
The Bias Blind Spot represents a discrepancy in recognition of cognitive bias — the difference between one’s self-perceived objectivity and the reality of one’s own biases. Cognitive biases represent a systematic pattern of deviation from norm or rationality in judgment, wherein subjective reality, through the filter of personal experiences and preferences, shapes and distorts objective…
Stereotype-linked Facial Features Prompt Perception of Social Class
A potent hierarchy, social class determines a variety of advantages and disadvantages in society. Existing research indicates that individuals form rapid judgments regarding the social class status of others, which can have significant ramifications. However, the precise factors that influence these judgments and their connection to assessments of beneficial or detrimental stereotypes remain unknown. In…
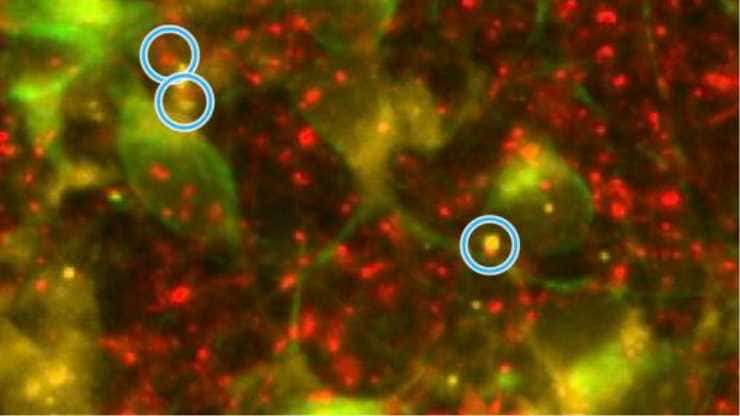
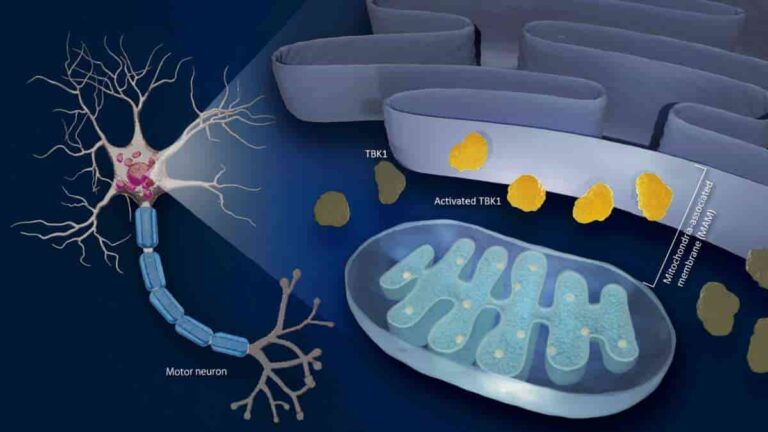
Disruption of Mitochondria-associated Membranes Linked to ALS Progression
Nagoya University researchers have identified a link between the progression of amyotrophic lateral sclerosis (ALS), also known as Lou Gehrig’s disease, and the disruption of mitochondria-associated membranes (MAM), the cell’s contact point between the mitochondria and the endoplasmic reticulum (ER). The finding provides important data about the mechanisms behind this neurodegenerative condition. Motor neurons are…
Social Media Use Predicts Higher Levels of Inflammation
With a thorough new study that demonstrated the same association over time, a social scientist at the University at Buffalo has expanded on a body of work that has previously suggested a link between social media use and inflammation. The findings raise intriguing questions about the nature of social media use and what may be…