The fundamental attribution error (FAE) is a cognitive bias that plays a significant role in social psychology. It refers to the tendency of individuals to overestimate dispositional factors, such as personality traits, while underestimating situational factors when trying to explain other people’s behaviors. This cognitive bias, also known as correspondence bias or attribution effect, was initially introduced by Lee Ross, a…
Difference Between Cognitive Behavioral Therapy and Behavioral Therapy
Cognitive Behavioral Therapy (CBT) and Behavioral Therapy (BT) both aim to help individuals with mental health issues, but they differ in their approaches to thoughts and emotions. CBT focuses on identifying and modifying negative thought patterns and beliefs that contribute to emotional distress and maladaptive behavior, while BT primarily addresses specific behaviors and seeks to…
Serotonin Loss May Play Role in Early Alzheimer’s Stages Cognitive Impairment
Researchers from Johns Hopkins Medicine have found that relatively lower levels of serotonin in certain brain regions of adults with mild cognitive impairment (MCI) may contribute to memory issues, including Alzheimer’s disease. The results come from comparing PET scans of over ninety adults with and without MCI. These results add credence to mounting evidence that…
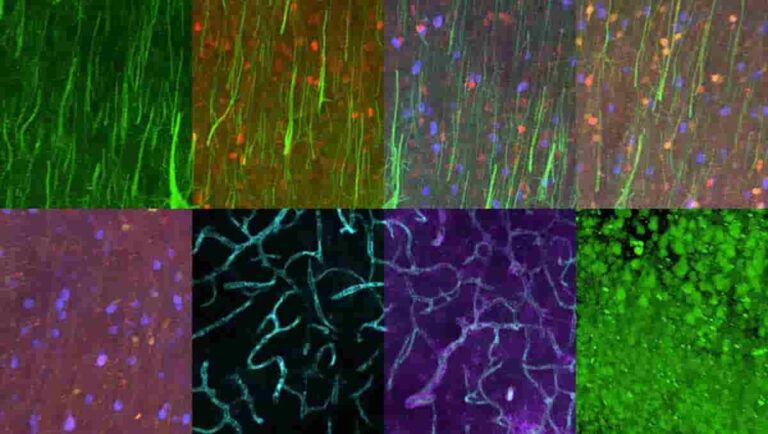
Protein Imaging Reveals Detailed Brain Architecture
MIT chemical engineers and neuroscientists have developed a new way to classify neurons by labelling and imaging the proteins found in each cell. This type of imaging offers clues to each neuron’s function and should help in mapping the human brain, the researchers say. Says Kwanghun Chung, who is the Samuel A. Goldblith Assistant Professor…
Parentified Youth – Impact Varies But Consequences Mostly Negative
We expect parents to take care of their children’s physical and emotional needs at all times. However, the roles are sometimes reversed, and the child takes on more responsibility than is acceptable for their age — a process called as parentification. For a variety of circumstances, adults may be unable to fulfill their parental responsibilities,…
Social and Emotional Development in Adolescence: Key Aspects
During adolescence, social and emotional development play a new role in an individual’s overall well-being. As adolescents navigate through this vital period of life, they acquire a greater ability to understand, experience, express, and manage emotions, as well as foster meaningful relationships with others. Adolescent development does not always proceed along the same course for…
TAF15 Aggregates Linked to Frontotemporal Dementia
The majority of neurodegenerative diseases, such as dementias, are caused by proteins that aggregate into filaments known as amyloids. Researchers may now target these proteins for diagnostic testing and treatment because they have discovered the proteins that aggregate in the majority of these disorders. However, scientists had yet to discover the rogue protein in approximately…
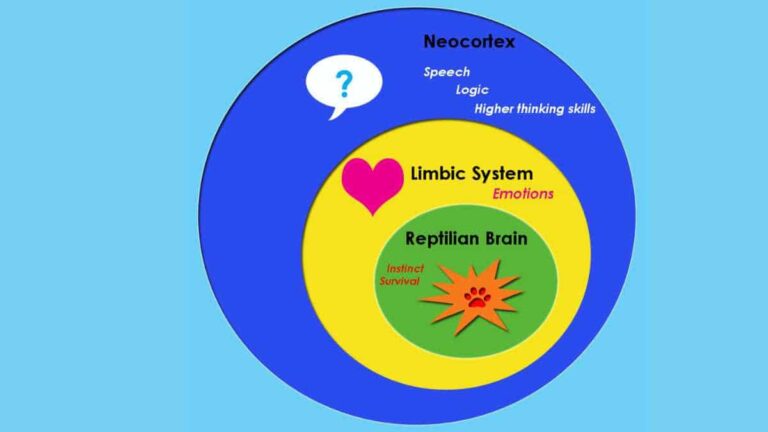
Is the Triune Brain Theory Still Relevant?
The Triune Brain Theory, developed by neuroscientist Paul D. MacLean in the 1960s, offers a simplified perspective on the structure and functionality of the human brain. This theory proposes that the human brain is composed of three distinct layers that evolved sequentially: Reptilian brain Limbic system Neocortex Each layer represents a different stage in the evolution of…
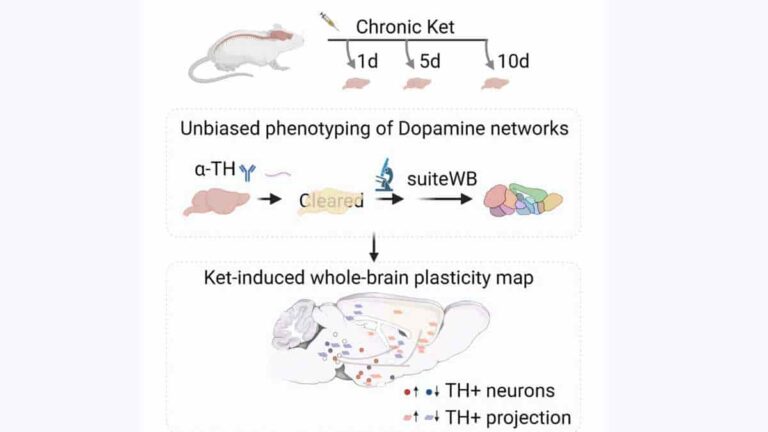
Restructured Brain Dopamine System Seen After Repeated Ketamine Use
Columbia University biologists and biomedical engineers traced ketamine’s effects on the brains of mice in a new study, discovering that repeated usage over long periods of time promotes broad structural changes in the brain’s dopamine system. The findings support the development of ketamine therapies that target specific areas of the brain rather than administering ketamine…