Artificial intelligence technology is being used to more accurately predict the risk of suicide in female patients with specific trauma-related disorders. The results of the three-year study represent a breakthrough in using AI to comprehend suicidal self-injury and could give clinicians a new way to quickly screen for warning signs.
The study was conducted by a team of researchers and clinicians from Worcester Polytechnic Institute (WPI) and McLean Hospital in Belmont, which is affiliated with Harvard Medical School. Information was gathered from 123 female patients at McLean Hospital, including 30 controls and 93 with histories of childhood abuse, PTSD, and varying degrees of dissociation.
The team created an algorithm that successfully predicted a patient group’s history of suicide attempts and pinpointed patient subgroups most at risk for suicidal thoughts and actions. Predictors included hearing voices, experiencing thought insertion, coming to awareness in the middle of an action the person does not remember starting, and finding objects in the person’s possession that they do not remember acquiring.
Twofold Approach
The team – led by Dmitry Korkin, professor of computer science at WPI, Lauren A. M. Lebois, director of McLean Hospital’s Dissociative Disorders and Trauma Research Program, and Suhas Srinivasan, a WPI doctoral student – used a dual strategy.
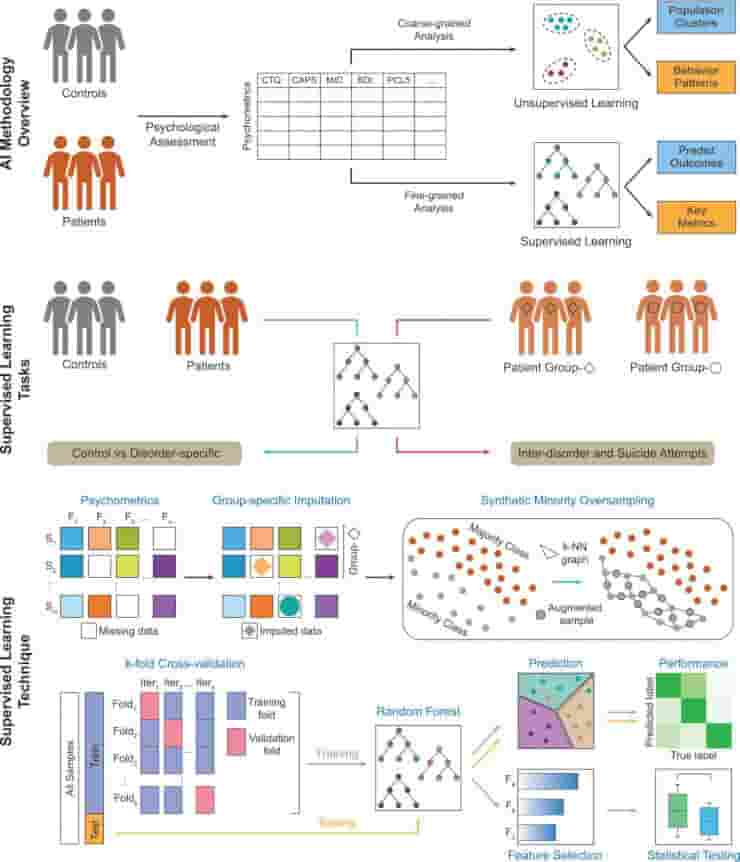
First, they clustered the data taken from the cohort using cutting-edge AI techniques created by Korkin’s team to check for patterns. The team used that information, according to Korkin, to identify distinct patterns in the patient population.
These patterns identified a range of dissociative symptoms that were associated with prior suicide attempts, such as a detachment from one’s self or from their surroundings, usually in response to trauma.
Second, the team developed an algorithm to distinguish between patients with various degrees of dissociation and the 30 healthy control participants in the study. The team also succeeded here, as the algorithm correctly predicted prior suicide attempts among the study participants in 83% of cases by focusing on particular dissociative symptoms as key indicators.
Finding Dissociative Identity Disorder Symptoms
AI and machine learning have previously been used to predict self-injurious and suicidal behaviours, but dissociative identity disorder (DID) has been understudied and underdiagnosed in general psychiatric practice and had not yet been considered in those models until now, according to Korkin.
He stated that the study highlighted the urgent need for clinicians to assess for dissociative disorder symptoms in order to identify high-risk individuals, particularly women, who are often overlooked in the study of suicide because they are statistically less likely than men to attempt suicide.
“We’re trying to say that among these hundreds of symptoms and indicators, our results suggest these two or three symptoms may be helpful to focus in on,”
Korkin said.
DID, like PTSD, covers a wide spectrum — people affected may exhibit some but not all symptoms, according to Benjamin Nephew, a neuroscientist and professor of biology and biotechnology at WPI who served as the team’s project coordinator. In the McLean/WPI study, a few of those dissociative identity disorder symptoms were associated with patients who had a history of suicidal ideation.
This could allow clinicians to focus more urgently on those symptoms when assessing a patient’s risk of suicide.
Significant Advance
The study’s findings could eventually lead to quicker referrals to dissociative disorder specialists and a greater understanding of how to use dissociative disorder diagnoses and treatments to inform suicide prevention.
“Interventions help with different things. Say, for example, you have depression and insomnia. Not everyone who has depression has insomnia, but if you do have insomnia with depression and you focus on that insomnia, it’s very effective at treating the depression,”
Nephew said.
Harry Kasparian, a 1973 WPI graduate, spearheaded this groundbreaking project in memory of his daughter, Julia, who committed suicide at the age of 23 in 2016. The Julia Kasparian Fund for Neuroscience Research funds collaborative research between WPI and McLean faculty and student neuroscientists, clinicians, and computer scientists to improve mental illness prevention, early diagnosis, and treatment, with a focus on DID, depression, and suicidality.
“This research represents a significant advance towards our objective of identifying patients at greatest risk of suicide and directing effective therapies at those individuals,”
said Jean King, a neuroscientist and the Peterson Family Dean of Arts and Sciences at WPI, who also worked on the study.
The team now intends to improve on these models and use them in future studies, broadening the coverage to other populations prone to suicidal ideation and behaviour. Clinicians may find the algorithm and its results to be useful in making a diagnosis.
“It’s the perfect case for an AI approach, which essentially is designed to get all the clinical data together, and then sift through it, ending up with a small number of clinical symptoms. We know that suicidal self-injury is complex and there is no one approach that fits every case. However, despite this complexity, we can still work to improve our ability to assess it,”
said Korkin.
Reference:
- Suhas Srinivasan, Nathaniel G. Harnett, Liang Zhang, M. Kathryn Dahlgren, Junbong Jang, Senbao Lu, Benjamin C. Nephew, Cori A. Palermo, Xi Pan, Mohamed Y. Eltabakh, Blaise B. Frederick, Staci A. Gruber, Milissa L. Kaufman, Jean King, Kerry J. Ressler, Sherry Winternitz, Dmitry Korkin & Lauren A. M. Lebois (2022) Unravelling psychiatric heterogeneity and predicting suicide attempts in women with trauma-related dissociation using artificial intelligence, European Journal of Psychotraumatology, 13:2, DOI: 10.1080/20008066.2022.2143693
